Over 90% of anal fistula cases require surgical treatment, according to NCBI. Non-surgical methods apply only in limited, early-stage conditions with strict medical criteria. Less than 10% of fistulas close without surgical intervention, based on Mayo Clinic evidence. Persistent infection and tract formation prevent natural healing in most patients.
Fistula surgery doctor in Delhi evaluate fistula type, infection depth, and recurrence risk before recommending treatment. Non-surgical approaches include antibiotics, drainage, and seton placement, but these methods do not eliminate the fistula tract. Treatment decisions depend on classification, symptoms, and progression timeline. Early symptoms such as pain, swelling, and discharge often indicate underlying abscess formation, which progresses to fistula in over 50% of untreated cases.
This guide explains when fistula treatment without surgery is possible, when it fails, and what treatment options are available in Delhi based on clinical evidence.
Fistula meaning in Hindi
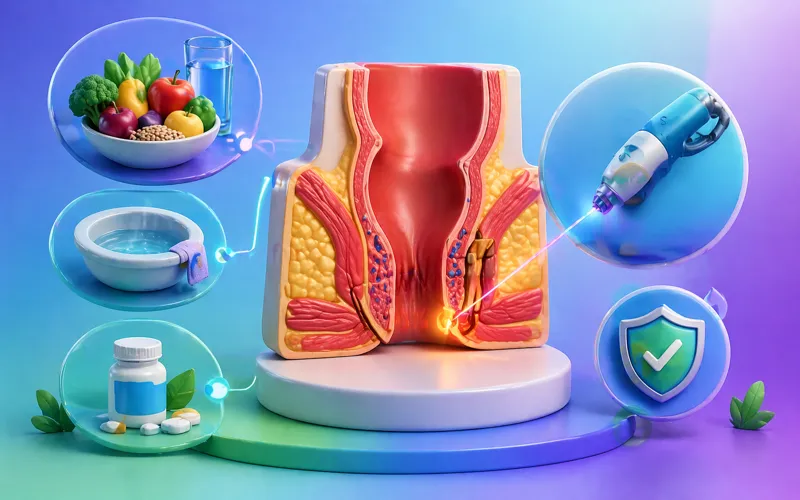
Anal fistula is an abnormal tunnel between the anal canal and skin near the anus. In Hindi, it is called “भगंदर (Bhagandar)”. It develops after infection in an anal gland that forms an abscess and creates a tract that drains pus or fluid.
Bhagandar is classified as a chronic condition because the tract does not close naturally in most cases. Medical literature describes it as a persistent connection requiring medical intervention when infection continues or recurrence occurs. In simple terms, it is a “pipe-like pathway” formed under the skin that keeps re-opening and draining.
Fistula symptoms and early signs in patients

- Initial symptom: persistent pain near anus
Pain is one of the earliest signs of fistula formation. It typically starts after an anal abscess episode. Clinical data shows that untreated abscesses progress to fistula in more than 50% of cases (NIH). Patients in Delhi often report pain while sitting or passing stool. - Swelling and redness near anal opening
Inflammation appears due to ongoing infection inside the tract. The affected area may feel warm and tender. This stage indicates active infection that is not resolving naturally. - Continuous or intermittent pus discharge
Discharge is a key diagnostic sign of fistula. It may be foul-smelling and stain undergarments. This occurs when the internal tract drains infection to the skin surface. - Recurrent abscess formation
Repeated swelling with temporary relief after pus drainage suggests a chronic fistula pathway. This cycle indicates that the underlying tract remains untreated. - Skin irritation and itching
Ongoing discharge causes irritation of surrounding skin. Patients often experience discomfort due to moisture and infection exposure.
Fistula types and classification
- 4 main clinical types classify anal fistula based on tract pathway: intersphincteric, transsphincteric, suprasphincteric, and extrasphincteric. This classification is used in surgical decision-making in Delhi hospitals to assess complexity and treatment choice.
- Intersphincteric fistula forms in ~60% of cases in clinical studies: the tract runs between internal and external sphincter muscles. It is considered the simplest form and has higher suitability for conservative or minimally invasive procedures in early stages.
- Transsphincteric fistula crosses both sphincter muscles: this type is more complex and carries higher risk of recurrence if not fully treated. It often requires surgical intervention due to deeper tissue involvement.
- Suprasphincteric fistula extends above the puborectal muscle: this structure increases surgical difficulty and reduces success rates of non-operative management.
- Extrasphincteric fistula bypasses the sphincter mechanism entirely: this type is rare and often associated with trauma or secondary disease such as Crohn’s disease, requiring specialized surgical planning.
Non-surgical fistula treatment in Delhi options
- Antibiotic therapy for infection control (temporary relief only): Antibiotics are used in early infection stages to reduce bacterial load and control pain. Clinical evidence shows they do not close the fistula tract permanently because the underlying tunnel remains open. This is why recurrence is common once medication is stopped.
- Seton placement technique (minimally invasive option): A seton is a surgical thread placed inside the fistula tract to allow continuous drainage. It reduces abscess formation risk and prepares the tract for later definitive treatment. In Delhi hospitals, it is commonly used for complex fistulas where immediate surgery is risky.
- Fibrin glue injection (limited success rate): This method attempts to seal the fistula tract using biological adhesive. Studies show variable outcomes, and success rates are lower in long or branching fistulas. It is generally suitable only for simple, early-stage cases.
- Fistula plug procedure (biologic closure method): A biocompatible plug is inserted to block the tract. While minimally invasive, recurrence rates are higher compared to surgical procedures, especially in high or transsphincteric fistulas.
- Laser-assisted treatment (FiLaC technique in select Delhi centers): Laser energy is used to destroy the epithelial lining of the tract. It is less invasive than open surgery but requires strict case selection based on fistula type and depth.
When non-surgical fistula treatment in Delhi fails
Persistent fistula tract remains open despite medication: When antibiotics, drainage, or fibrin glue fail, the epithelial lining of the fistula remains intact. This is the primary reason non-surgical treatment fails in most moderate and complex cases. Repeated abscess formation indicates treatment failure: If swelling and pus accumulation return after temporary relief, it suggests the internal tract is still active. In Delhi patients, this pattern is commonly seen in untreated or partially treated transsphincteric fistulas.
Incomplete drainage leads to chronic infection: Non-surgical methods may reduce symptoms but often fail to eliminate deep infection pockets. This allows bacteria to persist and re-trigger inflammation cycles. High recurrence after temporary closure methods: Procedures like glue or plugs can initially close the tract but show recurrence rates in clinical studies due to movement, infection, or incomplete sealing of branches.
Progression risk increases without surgical intervention: According to top surgeons in Delhi, delayed surgical treatment can lead to deeper tract formation and higher complexity classification, making future treatment more difficult and increasing recurrence risk.
Fistula is a chronic anorectal condition where an abnormal tunnel forms between the anal canal and surrounding skin. Non-surgical treatments such as antibiotics, seton drainage, fibrin glue, or laser-based procedures may be useful in selected early or low-grade cases. However, studies consistently show that recurrence rates remain significantly higher when the fistula tract is not fully removed or closed.
If you are experiencing persistent symptoms such as pus discharge, pain near the anal region, or recurrent swelling, early evaluation is important to avoid complications.
At Primus Super Speciality Hospital fistula cases are assessed using advanced diagnostic methods including imaging and clinical grading to determine the most effective treatment approach.
Book a consultation at Primus Hospital, Delhi for expert evaluation and personalized fistula treatment planning.